|
This
is a contribution from a member of THINCS,
The International Network of Cholesterol Skeptics
 Home
Home
Nov
14, 2003
WHAT
PROTECTS THE FRENCH FROM HEART DISEASE?
It's Not What You Think!
However
you look at heart disease, those pesky French throw a huge spanner in the
works. They should get heart disease, and they don’t, at least they
don’t get very much; about one quarter the rate in the USA and UK, despite
virtually identical ‘classical’ risk factors. This was first noticed by
Hugh Tunstall-Pedoe in 1978. He called it the ‘French Paradox,’ a term
that flits in and out of favour.
But
what are the French figures exactly? I think they are worth looking at
because they are extremely interesting. However, rather than looking at the
figures in isolation, I think it is a good idea to compare France with
another country, to highlight the almost perfect disparity between the
French risk factors and their rate of CHD.
The
best country to compare with France directly, is Britain, as these are two
countries that have virtually the same population, and GDP, and are
geographically very close. This removes a few variables.
The
figures I have used come from the British Heart Foundation and the BMJ.
CLASSICAL
RISK FACTORS vs. HEART DISEASE
(UK & FRANCE MEN AGED 45 - 64)
Average
total cholesterol level
France
6.1mmol/l
UK 6.2mmol/l
Average
HDL ‘good cholesterol’
France
1.3mmol/l
UK 1.3mmol/l
Average
systolic blood pressure
France
150mmHg
UK 148mmHg
Average
body mass index (BMI)
France
26.6kg/m2
UK 26.6kg/m2
Rate
of smoking
France
33%
UK 29%
Consumption
of saturated fat % of calories
France
25.7%
UK 27.0%
Rate
of type II diabetes (amalgamation of a number of studies)
France
~2.0%
UK ~2.0%
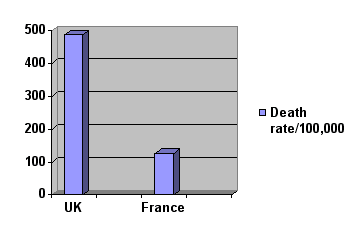
Death
rate from CHD ICD 414 classification
France
128/100,000/year
UK 487/100,000/year
Now
that’s what I call a paradox.
In
truth, I don’t call it a paradox at all. Because a paradox is an
apparently inexplicable finding for which there really is an explanation -
if only we could find it. This is akin to the wobble in the orbit of Neptune,
inexplicable until it was realised that there was another planet out there.
But
if you don’t believe that the classical risk factors are that important in
CHD, then you aren’t looking at a Paradox at all. What you are looking at
is proof that the generally accepted risk factors can only play a minor part
in causing CHD. As Magritte would say ‘ce n’est pas un paradox.’
RATE
OF DEATH FROM CHD MEN
AGED 45 - 64 (France vs UK)
However,
so deeply ingrained is the belief in classical risk factors that this
apparently contradictory evidence had to be explained away; a reason for the
low rate of CHD in France had to be found, one that did not damage the
current orthodoxy.
You
may ask why, when confronted with these two choices, the preferred option
was to look for a French protective factor, rather than a UK ‘killing’
factor? There are two or three interconnected reasons. But the main one is
that the British rate of CHD is roughly what you might expect from their
level of risk factors, in relation to other countries - give or take a
hundred per-cent or so either way. But the French rate stands out like a
sore thumb. It is a country with a high level of risk factors, and a very
low rate of CHD. Sixty million living, breathing, contradictions.
And
so, confronted with these facts, a desperate scramble began to find out what
was protecting the French. What do the French do, it was asked, that is
different from the British? Well, of course, they drink lots of red wine,
eat lots of garlic and lightly cook their vegetables (thus retaining
essential anti-oxidants). And by a remarkable coincidence, these three
things were then found to be protective against CHD. Or were they?
For,
if you search the literature closely, four things emerge
1.
Alcohol does protect against CHD
2.
Red wine provides no more protection than any other form of alcohol
3.
Garlic does not protect against CHD
4.
Anti-oxidants do not protect against CHD
This
has never stopped people claiming that these three factors are protective.
But if you look at the data closely, the evidence vanishes into thin air.
I’m
not going into the studies here in any detail, but I would lay a small
challenge to anyone who doubts that what I am saying is true. If you can
find one single study that has demonstrated a significant reduction in CHD
mortality that is attributable to garlic, anti-oxidants or red-wine
consumption (rather than any other form of alcohol), then I will admit that
I got this seriously wrong. But I think you’re going to have to search
hard, because I looked at study after study and could find nothing.
One
caution, you will find plenty of evidence clearly demonstrating that these
three factors definitely have an impact on risk factors in the blood, such
as LDL and HDL levels, and these data have been extrapolated to make the
claim that they are truly protective. But a positive impact on
‘surrogate’ markers in the blood does not mean a reduction in mortality.
To
use an example in the same area, hormone replacement therapy (HRT) was
claimed to reduce the rate of CHD, primarily because it raised ‘good’
HDL levels. This became far more than just a hypothesis, it became accepted
medical orthodoxy, and millions of women were prescribed HRT for this very
reason. Until the clinical trials were carried out, which have all clearly
demonstrated that HRT increases the risk of death from CHD - despite raising
HDL levels. (Which should tell you something very important about the
currently accepted risk factors, but I’m not going down that route this
time.
Moving
back to the French ‘protective’ factors for a moment. Look, for example,
at Garlic. The main reason why it is supposed to protect against CHD is
because it lowers cholesterol levels. But the average cholesterol level in
the UK and France is identical. So, how does garlic protect against CHD? By
lowering cholesterol levels you fool. But I thought you said the average
cholesterol level in the UK and France was the same. Repeat these sentences
until reduced to a gibbering wreck.
The
basic fact is that, when you look at the ‘supposed’ French protective
factors in any detail, you can find all sorts of evidence that they have a
beneficial effect on risk factors in the blood. Paper after paper, enough to
stretch to the moon and back. However, what you will not find amongst this
endless stream of data is any evidence of reduced mortality or morbidity.
Which is kind of important.
In
short, when you cut through all the hype, there are no such things as French
‘protective factors’, which means that there is no explanation for the
400% difference in the rate of CHD between the UK and France. A bit of a
gaping hole, I would vouchsafe. One that has not yet been filled.
Mind
you, on the surface, the theory that social dislocation causes CHD doesn’t
explain the low rate of CHD in France either. The total number of immigrants
living in the UK and France is almost identical. About four million in each
country, both of which have a population of nearly sixty million.
Internal
migration, from region to region, is also very similar. And when it comes to
general stress, the French take far more anxiolytics (anti-anxiety drugs)
than the British. Whether or not this means anything much, other than a
cultural phenomenon whereby the French are keener on taking drugs, is open
to debate.
Overall,
however, there appears to be nothing at all to explain the low rate of
French heart disease, either within the classical risk factors, or the
emigration/social dislocation model. Or is there?
Here
is where I return to a thought that I had twenty years ago, and which
triggered my lifelong interest in heart disease. I was at a meeting where a
study was presented which showed that rabbits who were fed in a less
stressed fashion - by a technician who liked rabbits; had less arterial
disease than rabbits fed by another technician - who didn’t think much
about rabbits one way or another.
Aha,
I thought, so unstressed eating may protect against CHD? If this is also
true of humans, I speculated, then populations where eating is an important
part of family life should have a low rate of heart disease; on the other
hand fast food cultures will have a high rate of CHD. A bit of a leap I
admit, but an interesting thought to pursue?
So,
I looked around the world at eating habits, and ended up focussing on
France. If one thing above all stands out about French culture, in relation
to British culture, it is their attitude to food and eating. The average
Brit treats meals as a refuelling exercise, the French, most clearly, do
not. They spend hours eating meals, relaxing, enjoying the food. It is a
social occasion.
I
began to wonder it were really possible that the French way of eating
protects them against CHD? If so, how? What is the biological explanation?
And can this possibly be related to emigration/social dislocation and
stress.
I
won’t bore you with the entire journey, but it comes down to this. From a
metabolic perspective the body is either in an anabolic state: eating,
digesting and storing food; or it is a catabolic state: rushing about, using
up energy.
The
hormones that switch on catabolism are the stress hormones: adrenaline,
growth hormone, glucagon and cortisol. The hormone that switches on
anabolism is insulin; and insulin and the stress hormones are direct
antagonists in many organs. Insulin switches off sugar production in the
liver, stress hormones switch it on. Insulin makes fat and muscle cells
absorb sugars and fats. The stress hormones do the opposite.
It
is apparent, therefore, that if you eat whilst under stress you will be in a
conflicting state of raised insulin levels, and insulin resistance. Just to
look at what happens in this state to the simplest metabolic substance,
sugar.
When
you eat sugar, it is rapidly absorbed, the level in the bloodstream rises,
and insulin is released, causing the blood sugar level to drop. But if you
are stressed, glucagon and cortisol will be trying to drive the sugar level
up. In this situation, what can the metabolic system do? It will keep on
cranking up the insulin levels to overcome the resistance to insulin,
however, in most cases this is still not sufficient to overcome the
resistance.
So
what you will see in a person eating sugar whilst stressed is a combination
of three things:
1.
A raised level of stress hormones
2.
A raised level of insulin
3.
A raised blood sugar level
All
of these things damage the endothelium. Raised stress hormones also increase
blood coagulability. In addition, hyperglycaemia induces a state of
oxidative stress (release of free radicals) which stimulates platelets to
stick together, which also creates oxidised LDL - both of which further
promote thrombus formation
Thus,
eating under stress creates the exact metabolic state, pro-coagulant state,
that leads to endothelial damage and thrombus formation. I believe that this
damage is the underlying cause of atherosclerotic plaques and premature
death from heart disease.
Any
proof of this? Well, the truth is out there.
Just
to look at two studies. In the first study healthy volunteers were given
stress hormones in levels designed to mimic post-aggression metabolism (PAM).
This is a metabolic state that occurs when the body is damaged through some
form of ‘aggression,’ a road traffic accident, surgery etc.
In
this study, in those given the stress hormones, insulin sensitivity was
reduced by 88% (A state of severe insulin resistance). And when they were
given a glucose infusion, insulin and sugar levels sky-rocketed Heise T
Metabolism Oct 1998
1.
The peak insulin level was 352 pmol/l vs 110pmol (or, approximately
three times as high as in controls))
2.
The peak sugar level was 19.7mmol/l vs 7.2mmol/l (or, approximately
three times as high)
So,
it is clear that a high level of stress, and stress hormones, in conjunction
with food, creates exactly the metabolic state that triggers atherosclerotic
plaque development.
But
can transient mental stress, rather than the physical stress of the
post-aggression state, also cause insulin resistance. Indeed, it can.
‘It
is concluded that acute mental stress induces a state of insulin resistance
in IDDM patients, which can be demonstrated by an IGIT (insulin, glucose
infusion test) to appear 1 h after maximal stress and to last more than 5
h.’ Moberg E Diabetologia Mar 1994
In
short, both mental and physical stress can induce a state of insulin
resistance, resulting in a form of transient syndrome X. So it becomes very
clear that the basic mechanism by which eating under stress causes CHD is
exactly the same as the state induced by emigration/social dislocation. The
only difference is that eating under stress is a transient state,
non-detectable when fasting, which is, as you may well have noted, when the
vast majority of tests are carried out. So it is not surprising that no-one
has spotted this yet.
Anyway,
to return to the question posed in the title of this article. What protects
the French? I think it is clear that they are protected not by what they eat,
but by how they eat. By eating in a relaxed fashion they do not pit the
system of anabolism and catabolism against each other, they do not trigger
insulin resistance, and hyperglycaemic spikes, and therefore they do not
damage the endothelium in the prandial/post-prandial state. Vive la France!
Top
 Home
Home
|